08 Feb 2019
Parents question: Is doctor's help necessary if a person tries to quit drugs? It is not necessary, unless it has severe concomitant diseases (for example, heart or lung disease) or complications of addiction - thrombophlebitis, phlegmon, convulsive seizures, etc. On the other hand, if the promise of medical assistance helps the drug addict to decide on treatment and you are of course, we should use this opportunity.
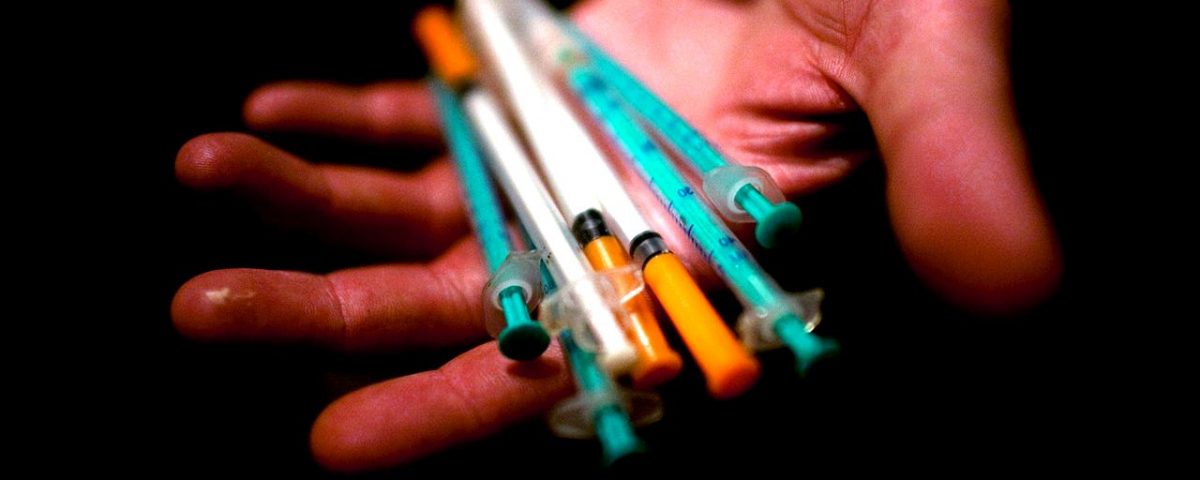
The first way to treat drug addiction, which comes to the head of the addict himself is to alleviate withdrawal with the help of various medications. He reasons this: "The most important thing is to going cold turkey, and then I will not just take drugs."
What medicines does the addict choose for self-treatment?
1. Sleeping Pills
2. Painkillers
3. "For the liver." (Heptral etc)
As drug addicts feel ill during the treatment, they are habitually trying to "disconnect" from their poor health. The most suitable from their point of view for this tool are sleeping pills, which they are ready to use in incredible quantities. And the most popular in their environment are the strongest drugs. Currently, almost the only means for self-treatment addicts consider Phenazepam or reladorm - a combined hypnotic drug in the form of tablets containing cyclobarbital. Cyclobarbital refers to the hypnotic barbiturate series and, like other barbiturates, is able to form a real drug addiction. In addition, it is with massive use (namely, so it is used by drug addicts) causes brain damage - encephalopathy.
But that's not all
If in the treatment of abstinence syndrome ("cold turkey") the rate is to be made only for sleeping pills - even not for reladorms, then this treatment may not end in anything. The fact is that the addict takes sleeping pills to "not feel broken". But as soon as he wakes up, unpleasant symptoms arise with renewed vigor. He again takes an increased dose of sleeping pills (the normal dose does not cause sleep during the abstinence period). And so a few days (from 7 to 14) in a row. As a result of an overdose of sleeping pills, poor state of health persists, although abstinence ("withdrawal") has already subsided. And the more the dose of sleeping pills, and the reception of them longer, the worse the condition becomes. True, this situation is typical only for drug addicts with a relatively long experience of narcotics, but in 50% of cases of self-treatment attempts and even more often this is what happens.
Parents question: How to deal with sleep disorders in a drug addict? While he uses drugs, it is better not to fight. The problem does not completely solve all the same, and the regular use of sleeping pills worsens the prognosis for recovery. When he stops anesthesia, this question should be addressed to a doctor. In general, during this period, a hot bath or shower at night helps, if sleep disorders are not too pronounced.
As an anesthetic, first of all, the addict tries to choose opiate drugs - for example, methadone. He tells his family that other drugs do not completely "relieve" the pain and do not help fall asleep (and this is true). The result of such "treatment" is usually the transition to another drug, often more dangerous and expensive. Therefore do not agree with this method of "treatment".
Parents question: Should I use analgin, pentalgin, reladorm during abstinence? Analgin is not absolutely safe drug - in large quantities it damages the heart muscle. In addition, its effectiveness with abstinence is usually low. Pentalgin and reladorm contain barbiturates, which in themselves are drugs and cause damage to the brain.
So think ...
In recent years, there are two effective publicly available analgesics, and since drug addicts still use them spontaneously, I will also say a few words about them.
The first is called "tramal" and is sold in ampoules, capsules, candles and drops. It helps well from toothache, but in healthy people (especially women) it often causes nausea. It costs expensive. In itself, during abstinence, drug addicts help badly. Doctors use it, but in combination with other drugs and quite a limited time. If you use tramal for several days, its effectiveness drops dramatically.
The second drug is called "ketorol" (sometimes "ketanov") and is sold in tablets and ampoules. Its advantage over tram is that it is sold without a prescription. It is relatively expensive. You can take only after eating. During abstinence drug addicts help badly. We use it, but only when the "breaking" is already on the wane. If applied more than 5 days in a row, it can cause a stomach ulcer; therefore it is contraindicated in those who have already had it.
Only in occasion of reception of preparations "for a liver" - Essentiale, karsil, Heptral, Layennec, etc. - I can not say anything bad. Of course, they are shown to most drug addicts, especially those who use "intravenous" handicrafts. But I advise you to consult your therapist at your place of residence - just not to overdo it with the dose.
Of course, one can not expect that these drugs will help a drug addict to quit drugs
As you can see, I am skeptical about self-medication with the help of pharmacological agents. But there are other ways to help yourself. And I am glad to welcome them with all my heart:
1. "Breaking into dry" - that is, without the use of medicines. This method can be used by 95% of drug addicts without serious risk to themselves. This is dangerous only for those who suffer from severe chronic diseases such as ischemic heart disease, liver cirrhosis, chronic kidney failure, etc. Among drug addicts, such patients are found, but infrequently - usually die before they decide to be treated. But! Most drug addicts do not agree to transfer "breaking to dry" simply because of the fear of pain.
2. Use of a bath, a sauna and hot water procedures. The restrictions are the same as for "dry breaking", but the abstinence in the hot water is much easier to tolerate. A good physiological way, I would gladly recommend it to anyone who wants to give up drugs.
3. The same, but in the summer in the Sea. In conditions of constant high atmospheric pressure and relatively high air temperature, against the backdrop of mountains, green cypresses and the sea coast, you can abandon drugs almost painlessly. The method is good for those who have money and time.
4. Refusal of drugs on the background of religious enthusiasm, a very joyful, frightening or tragic event in life. In the conditions of a sharp, prolonged and violent change in the emotional background, "breaking" is almost not felt (for example, this happens when a drug addict has to hide from pursuit). The same is true of sudden spiritual enlightenment. So for those who have the strength to believe in God - this is a good chance to get rid of the drug addiction forever. In the jargon of narcologists such a method of detoxification is called "to break on the holy spirit." In the case of sincere faith, he works irreproachably.
5. Finally, giving up drugs after a long, serious illness. If the addict is in serious or even in a relatively serious condition due to pneumonia, pulmonary edema, heart attack, trauma, poisoning, etc. and at this time does not use drugs for at least five days - he can safely abandon them and in the future - "break" it will not.
There is another way to "cure" without drugs - to get to a prison where drugs can not be obtained. To my great regret, it is impossible to get rid of addiction as a state of mind in prison.


 Cart
Cart