Cirrhosis of the liver
11 Oct 2018
For the first time this term appeared in the literature in 1819. In our time, cirrhosis develops in 1-1.5% of the population of the Slavic countries. At what most often it is men in the age of 40 years. In 80-85% of cases, the main cause is alcoholism and viral hepatitis. Cirrhosis of the liver is a chronic liver disease that progresses rapidly and leads to the development of functional organ failure and portal hypertension (increased pressure in the system of vessels coming from the internal organs to the liver).
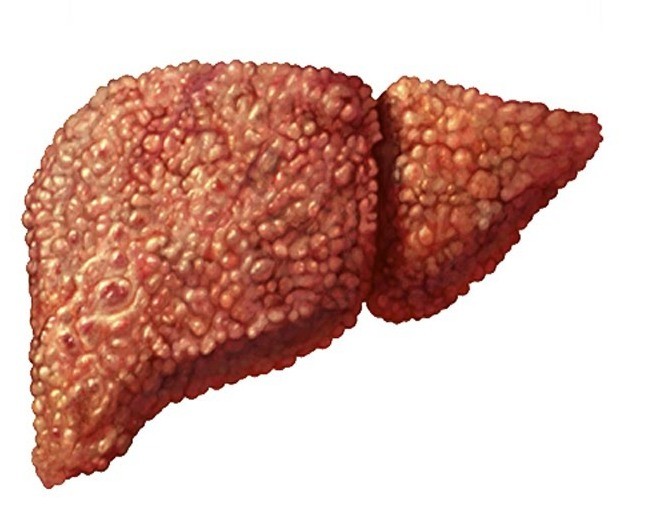
When cirrhosis is formed, the liver cells die and replace them with a connective tissue (similar to the scars on the skin), the blood vessels of the liver are modified. This leads to the fact that the liver stops performing its usual functions.
Stages of cirrhosis of the liver
Currently, there are several different classifications of liver cirrhosis, which are based on different aspects of the disease.
Classification by morphological features:
- Micronodular, or small-node cirrhosis - the diameter of the nodules varies in the interval 1-3 mm;
- Macronodular, or coarse nodular cirrhosis - diameter of nodules from 3 mm or more;
- Mixed cirrhosis - a combination of nodules of various shapes;
- Incomplete septal cirrhosis.
Classification of cirrhosis due to its occurrence:
- Viral cirrhosis - develops against the background of viral hepatitis B or C;
- Alcoholic cirrhosis of the liver - develops from long consumption of a large amount of alcohol, which first leads to fatty liver, followed by alcoholic hepatitis, and at the end - cirrhosis;
- Medicinal cirrhosis - arises from the long-term use of certain medicinal substances, which in large quantities can adversely affect the liver cell (for example, some antibiotics);
- Secondary biliary cirrhosis;
- Congenital - develops in children in the absence of bile ducts;
- Stagnant, cardiac cirrhosis of the liver - in case of circulatory failure, which arises in case of heart disease;
- Syndrome and Badd-Chiari disease - patients are concerned about pain in the liver area (under the right hypochondrium), abdominal enlargement, fever, minor jaundice, very large liver, lower edge painful, spleen slightly enlarged, frequent bleeding from esophageal veins. For this form, the defeat of the posterior surface of the liver and the changes in the vessels are most characteristic;
- Alimentary cirrhosis - with diabetes mellitus, obesity;
- Cirrhosis with an unclear reason:
Cryptogenic cirrhosis of the liver is extremely rare. But has a tendency to rapid development of clinical symptoms and the onset of complications. Is a direct indication for a liver transplant.
Children's Indian.
Primary biliary cirrhosis - the main complaints with this form are pronounced itching of the skin and intense jaundice, later the weakness in the whole body, weight and pain in the area of bones are added. Complications occur later than with other forms of the disease.
Classification by stages of cirrhosis:
- Compensated cirrhosis of the liver;
- Subcompensated cirrhosis of the liver;
- Decompensated cirrhosis of the liver.
Classification by clinical course:
- Subacute cirrhosis is a transient phase between hepatitis and cirrhosis. Lasts from 5 months to 1 year.
- Rapidly progressive cirrhosis - complications and a vivid clinical picture develop very quickly. Life expectancy is about 5-6 years after the onset of the disease.
- Slowly progressive cirrhosis - symptoms gradually develop gradually, and there is a long-lasting absence of complications. The duration of this variant of the disease is more than 11 years.
- Sluggish - there are practically no clinical symptoms, changes in the analyzes are minimal. The duration of this form is more than 16 years.
- Latent cirrhosis of the liver - there is no change in the analyzes, no complaints, and there are no complications. Life expectancy does not depend on this cirrhosis. The diagnosis is made by chance, when diagnosing other diseases.
An example of a diagnosis: cirrhosis of the liver in the stage of decompensation, micronodular, alcoholic etiology, grade C according to Child-Pugh, varicose veins of the esophagus of the 2nd degree, hepatic encephalopathy of the first stage.
Symptoms and signs of liver cirrhosis
Symptoms of cirrhosis include pronounced general weakness, unmotivated memory impairment, fever, pain in the right upper quadrant, weight loss, nausea, abdominal enlargement, dry skin.
The signs that the doctor discovers during examination include the enlargement of the liver and spleen, red palms, smooth and bright red tongue, vascular "sprouts", veins on the abdomen ("jellyfish head"), scalp and inguinal region, jaundice, various hemorrhages in the body, varicose veins.
Treatment of cirrhosis of the liver
The main measures for treatment include: remove the effect of the causative factor; compliance with diet (refusal of alcohol, from fatty, fried, spicy food, from certain food products); treatment of the disease that caused cirrhosis (sorbents, hepatoprotectors – Heptral, Layennec, detoxification therapy, antiviral and others- Phenotropil, Phenazepam).

 Cart
Cart